Application of a topical photoparticle immediately before non-ablative 810 nm diode laser treatment for acne resulted in a statistically significant reduction from baseline in inflammatory acne counts on the back, according to a small feasibility study presented in April at ASLMS.
Dermatology Times – Dermatology



Tag Archives: back
Prevent Back Acne (Bacne)
“Bacne”
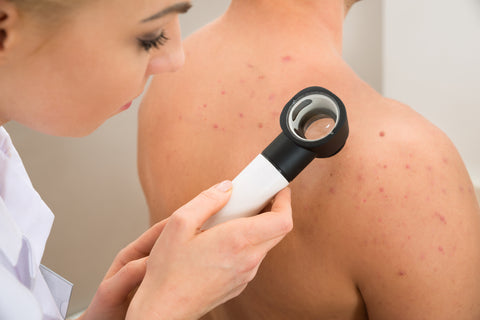
I don’t know about you but I had many friends growing up who suffered from back acne and seeing as my mom was a dermatologist would always ask me how I avoid it or how to get rid of it and I never really knew the answer, I just knew I was lucky that I didn’t have it! After sitting down with Dr. Norris I learned that some people are more prone to “bacne” than others and specifically there are two groups, people who sweat a lot such as athletes and then those with a genetic predisposition for acne. Meaning this condition has a hereditary property, so don’t forget to thank your parents next time you see them if you have breakouts on your back! But don’t start to worry yet because there is still hope as there are some ways to minimize breakouts on your back.
3 Tips for Minimizing Bacne
- Taking shower as soon after exercises or physical activity can help prevent breakouts

- Try to get out of your sweaty clothes as soon as possible after exercise. A lot of times people go to a work out class or on a run then head to meet up with friends, but staying in your sweaty clothes can impact your skins health and cause breakouts. If you don’t have time to shower, at least change!

- Using benzoyl peroxide to treat this condition but you want to be very careful when using benzoyl peroxide as it can bleach your clothes and towels. Dr. Norris suggests putting it on directly after bathing and letting it dry completely before putting on your pajamas or climbing into bed!

- Finally, it is sometimes helpful to wash your back once a week with a medicated shampoo such as Selsun blue shampoo.
While some of these preventative measures can help minimize breakouts typically a dermatologist should see this condition, as a common treatment is an oral antibiotic along with a good skincare routine. Acne on the back does not tend to respond as readily to topical treatments as the inflammation is deeper in the hair follicle on the back than say acne is on the face.
Amanda Blakley Skincare – BLOG
Yoga and Lower Back Pain
In a recent study published in the Annals of Internal Medicine, Boston Medical Center researchers found that yoga classes specifically designed for chronic lower back pain (my italics!) helped patients feel better. In light of this those with non-specific Lower Back Pain might also be interested in this podcast which features Stuart McGill (regarded as the God of Lower Back Pain) discussing yoga and lower back pain
The post Yoga and Lower Back Pain appeared first on Whole Life Fitness.
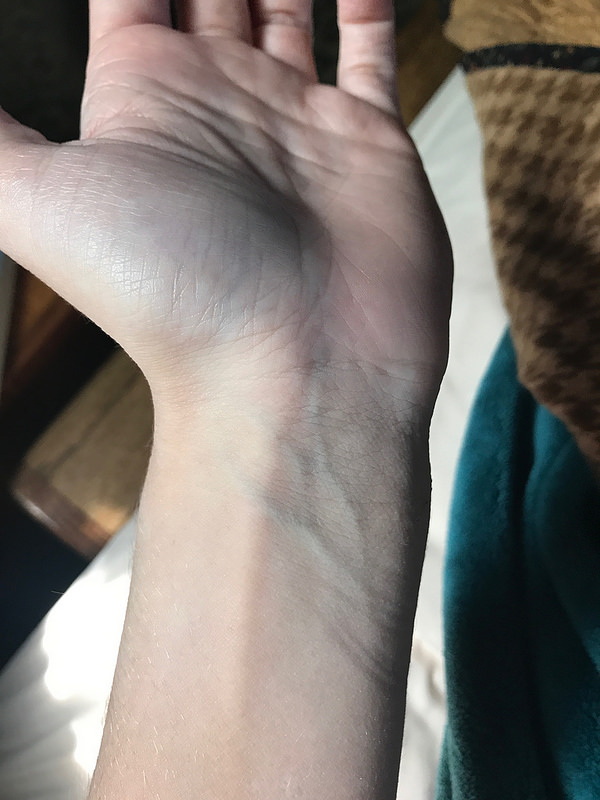
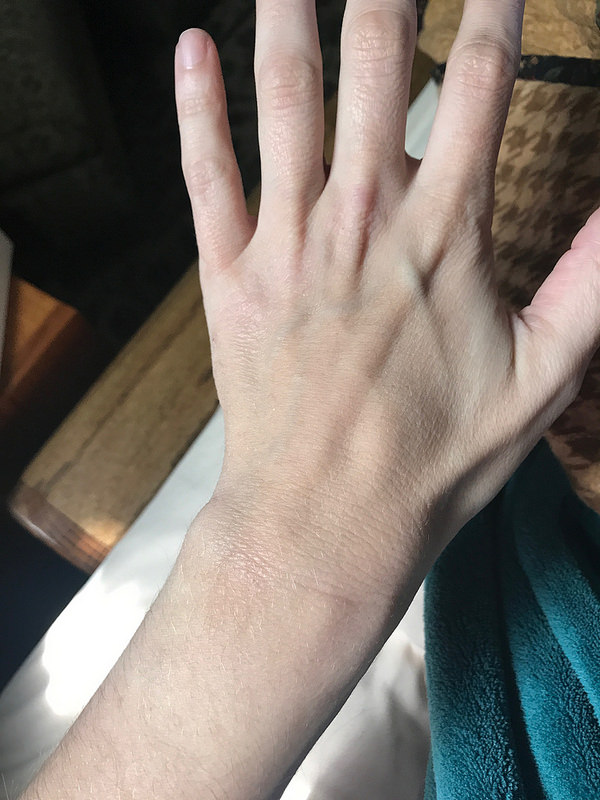
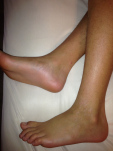
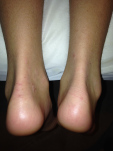
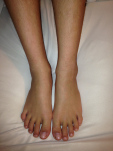
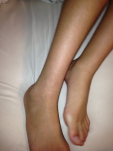
TSW to Dr Aron’s… ZERO regret and I gained my LIFE BACK!!!
Good grief! I don’t even know where to start. I stopped blogging because, honestly, I didn’t have time. My life has been so full and back to normal along with my skin that I haven’t had anything to blog about. I don’t take photos of my skin anymore. I don’t have updates. I’m just back to living my life without thinking about my skin. Skin no longer dictates everything I do. Showers feel great. I sleep through the night without Benedryl. I have energy. I am eating more foods! ALL good. How? Well, some of you are going to cringe when I say this and quite frankly I just don’t care. I spent my WHOLE TSW experience trying to bring hope to the people who were in the depths of hell. Showing them where I’d been and how much healing I’d experienced. But, truthfully, after nearly 2.5 years of TSW hell, I could no longer convince anyone, including myself, that time was going to heal me. I needed to get back to my life. I needed to focus on my kids and my family. I needed SOMETHING. Enter, Dr. Aron.
After 3 days I could shower! Showers were no longer EXHAUSTING. They took everything out of me! It was so awful! Well, after just days, showers felt amazing. I remember standing in the shower with tears of joy streaming down my face because it felt like a shower. A beautiful, warm shower. No intense itching. No intense burning. No knife like cut feelings. Just wet warmth. I had suffered for 2.5 years. Even avoiding showers for an entire year due to the HORRIBLE pain. You read that right, I didn’t shower for a YEAR. I am so mad even typing that.
After a few weeks I could sweat without feeling the heat flare! Oh the freakin heat flares! I would know I was sweating before I was even sweating because the itch would start. The slightest raise in heat would cause my body to slightly perspire and the sweat would sting and burn all the broken skin. OMG it was miserable! I couldn’t work out, I couldn’t walk in the heat, I couldn’t do anything without feeling like I could just itch my skin off. UGH.
After 10 days I looked like I’d lost 10 lbs because the swelling had gone down so much. You could see my chin again.
It took much longer of the wrinkles to subside. That was months, really.
After 6 months I went on a date with my husband to a work Christmas party and TRULY felt beautiful. My skin played a huge roll in that.
Back in business: treatment options for lower and chronic back pain
While back pain can be debilitating and distressing, there are a number of treatment options available. As the largest private hospital group in the UK, BMI Healthcare are used to providing a range of options and treatments for back pain, read there article below and find out what you can do.
Intro
Each year, 1 in 3 people develop back pain(1). In most instances, people experience moderate pain in the lower back which can be managed with over-the-counter painkillers. Lower back pain is extremely common, affecting about 4 in 5 people at some point in their life, usually between the ages of 30 and 60. It can last days, weeks or even months. When pain continues for over three months, it becomes known as chronic back pain.
Back pain – especially chronic back pain – can affect people’s mood, sleep, work and quality of life. While it’s often difficult to identify the exact cause of back pain, it’s usually related to strained muscles, tendons or ligaments, or other structural damage.
Surgical and non-surgical treatment
The use of surgery to treat back pain is quite rare; there are a number of non-surgical treatment options available, and spinal surgery will usually only be offered as a last resort if these treatments prove ineffective.
Indeed, unless you have a condition that specifically requires surgical intervention, doctors are likely to recommend painkillers, psychological therapies, exercise and physiotherapy, acupuncture or pain management before they opt for surgery. The most common conditions corrected by spinal surgery include prolapsed discs, which cause nerve symptoms in the neck and back, along with chronic neck and back pain.
Types of spinal surgery
However, if surgery is required, there are several types of intervention to consider. Some interventions are intended to relieve back pain caused by wear and tear, while others target limb pain – for example, sciatica in the leg caused by nerve pressure in the spine.
Your GP will help to determine whether or not you require back surgery. If a disc in your back has become damaged and is putting pressure on the surrounding nerves – sometimes referred to as ‘a slipped disc’ – you could be offered a discectomy. This procedure involves removing the whole or part of one of the discs between your vertebrae.
For a condition known as spinal stenosis, which causes the space inside your spine to narrow, you may undergo a laminectomy. This involves removing a small part of the bone called the lamina at the back of your vertebra.
Spinal fusion, meanwhile, is a procedure to join two or more vertebrae together using bone grafts, rods and screws in order to strengthen and stabilise the spine and prevent pain caused by movement. A spinal fusion may be recommended if you have a condition such as spondylolisthesis, whereby one of your vertebrae slips out of place, or if you suffer from severe degenerative disc disease.
Damage to vertebrae can also be repaired using a procedure known as vertebroplasty, which involves injecting a bone-cement into the vertebra. This procedure is often used to treat compression fractures caused by trauma or osteoporosis(2).
Be prepared
The back is a complex structure made up of bones, muscles, ligaments, tendons, joints and nerves. The spine supports the back and is made up of 24 separate vertebrae; it also encases the spinal cord, which carries nerves from the brain to the rest of the body.
Surgical intervention in such a crucial part of the body is no small undertaking and not a decision that should be taken lightly. If it’s recommended that spinal surgery is the best course of action available to you, you must make all necessary preparations in advance of your operation.
While most people can walk after back surgery, in the first days after an operation simple, everyday tasks such as lifting, driving, washing, cleaning or dressing may be painful and problematic. You may want to ask a friend or family member to help you during this time. You’ll certainly need someone to pick you up from the hospital.
If you smoke, you may be asked to stop before your operation, as smoking increases the risk of chest and wound infection, which hampers the recovery process. In the hours before the operation, you’ll most likely be asked not to eat or drink as most back surgery involves a general anaesthetic. In addition, during your time in hospital you’ll probably be asked to wear compression stockings to help prevent blood clots forming in your legs.
A personal choice
Ultimately, the final decision to proceed with spinal surgery lies with you and you alone. Your doctor and surgeon will discuss the options with you, but if you decide not to go through with surgery then they will respect your wishes.
Furthermore, pain is personal and subjective, and the way in which it is treated is down to the preferences of the individual involved. Back pain can become debilitating and severely impact your quality of life; some people opt for surgery, while others choose to manage their pain through physiotherapy and alternative therapies, such as acupuncture.
Whatever route you select, it’s vital to ensure your treatment pathways not only give you a chance to live a life free of pain and discomfort, but that they are appropriate for you and that you are happy with the choices you make.
To find out more and discuss your options with BMI Healthcare please get in touch and make an enquiry.
(1) http://www.bupa.co.uk/health-information/directory/b/back-pain
(2) http://www.bupa.co.uk/health-information/directory/b/back-surgery
Back for Christmas
Maybe its the winter, maybe its the stress of Christmas approaching but either way the eczema is making a comeback.
The patch that started this blog is looking a bit red after being gone for months and there is a little patch on my right wrist.
Today I noticed about a 3″ cirular patch on the inside of my right elbow.
I’m guessing its to do with stress and I know what’s causing my stress at the moment, just not sure what to do about it…
Update: just as this batch came it has gone. In the last few days I have started getting an itch on right calve which I am using Eumovate on which should clear it up.
23 months TSW and back to school 2015
You know you’re a TSW-obsessed mama when your child’s 1st-day-of-school pictures look like this:
First day of 7th grade 9/8/15. Have a GREAT year, Brian!
“A longing fulfilled is a tree of life.” Proverbs 13:12